Inflammation During Menopause: Why It Happens and What to Do About It

Each stage of menopause – premenopause, perimenopause, and postmenopause – comes with changes inside and outside your body. And since menopause is a life stage encompassing a third of your life, it is a good idea to understand what’s happening to alleviate symptoms and lower your risk of chronic disease. One of the changes that can take place during any stage of menopause is an increase in inflammation. Read on to learn more about inflammation, how it is affected by menopause, and ways to prevent or decrease inflammation.
Inflammation 101
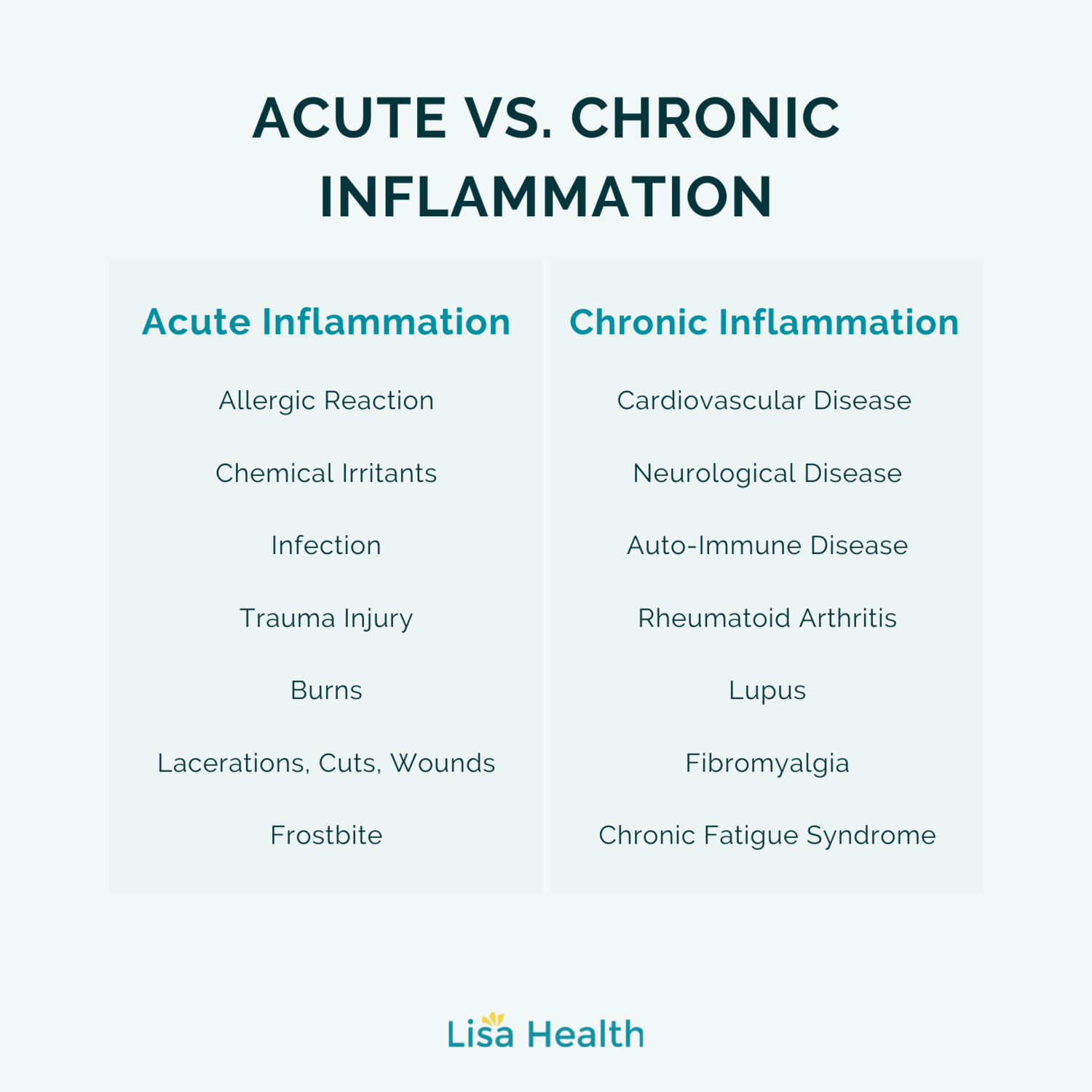
When you think of inflammation, it probably calls to mind red, swollen skin around an injury or something that happens when you are sick. Inflammation in these scenarios is a sign of your body doing its job in trying to fight off foreign invaders, like bacteria, viruses, and splinters. Inflammation occurs in response to an acute injury or infection when white blood cells are called to the site, eliciting a defensive response that causes inflammation due to the increased number of cells in the area.
There can be other causes of inflammation, such as menopause. The previous examples were of acute inflammation. But you can also experience chronic inflammation that can come from various health factors like smoking, poor diet, heart disease, arthritis, and even menopause. An acute infection or injury does not cause the type of inflammation associated with menopause. Still, both types of inflammation are similar in that they occur in response to an increased number of white blood cells in the body.
The Menopause-Estrogen-Inflammation Connection
There is plenty of research showing that inflammation can increase during menopause due to declining estrogen. Estrogen is anti-inflammatory, so it makes sense that as it decreases, inflammation increases. This change can occur during any stage of menopause. One study concluded that postmenopausal women had higher white blood cell counts, which indicated an association with increased chronic systemic inflammation. Similarly, another study from the Journal of Neuroinflammation found that estrogen decline during perimenopause is pro-inflammatory. This may be due to the release of inflammasomes, or cells that induce inflammation, from the ovaries as they transition.
Bottom line, midlife women going through menopause are likely to experience inflammation throughout their bodies due to estrogen decline. This onset of inflammation can be associated with a higher risk of symptoms like joint pain and certain health issues, like cardiovascular disease, cognitive decline and dementia, and even poor gut health.
The Relationship Between Menopause Symptoms and Inflammation
As noted above, inflammation caused by the stages of menopause can increase your risk of health issues and certain symptoms. For example, you may notice inflamed joints in your hands or other areas of your body. This inflammation can be accompanied by pain and is thought to be due to decreased estrogen. Some women also notice weight gain during menopause, especially in the belly area. Weight gain and inflammation are associated and as one increases so does the other.
A few other health issues can arise during menopause. As you begin going through menopause, your risk of Alzheimer’s disease increases. According to a study from Frontiers in Aging Neuroscience, estrogen acts as a potent anti-inflammatory agent. When it declines, inflammation increases, which is a factor in the onset and progression of Alzheimer’s disease. Plus, estrogen is thought to protect your brain from degenerative diseases and cognitive decline, which means you may experience changes in your cognition during menopause.
Gut issues can also begin during menopause. This study on sixty five midlife women concluded that inflammation in the gut increased from premenopause to postmenopause. Inflammation was associated with increased gut permeability, which may allow bacteria to leak through your gut, possibly explaining any new stomach issues you have during menopause.
Working on reducing inflammation may help alleviate menopause symptoms and other health issues.

Preventing Inflammation
Fortunately, there are simple strategies you can use to reduce inflammation in your body. There are both holistic solutions and medications that can help.
Holistic Solutions
- One of the most impactful changes you can make is to eat more anti-inflammatory foods and less inflammatory foods. For example:
- Anti-inflammatory foods: rich in fiber like fruits, vegetables, whole grains, and nuts, fermented foods like yogurt, kimchi, and kefir, healthy fats like fatty fish and olive oil
- Inflammatory foods: refined sugar and carbohydrates, highly processed foods, fried foods, red meat, trans fats
Learn more about which foods to eat and those to avoid with our anti-inflammatory food guide available in the Midday app.
- Consider taking a probiotic or adding more fermented foods to your diet. A study published in Cell found that eating six servings per day of fermented foods reduced systemic inflammation.
- Get regular exercise. It has been found in studies that regular physical activity can have anti-inflammatory effects.
- Reduce stress in your life. Consider practicing mindfulness, yoga, or other activities that will benefit your mental health.
- Be sure to get enough uninterrupted sleep. According to research, establishing a bedtime and sleep routine that ensures you get plenty of quality sleep every night can improve inflammation.
- Practice good oral hygiene. If your gums bleed when you brush or floss, that may be a sign of inflammation in the gums.
- Quit smoking. The toxins from smoking have a direct link to inflammation.

Medications and Prescriptions
- Hormone therapy may help reduce inflammation for menopausal women.
- One study found that daily use of hormone therapy reduced general inflammation in women within six years of menopause. This reduction in inflammation also reduced atherosclerosis or plaque buildup on artery walls.
- Another study concluded that women who started hormone therapy soon after menopause might improve their cardiovascular health by counteracting fluid retention and inflammation.
- Other anti-inflammatory medications, like NSAIDs, are available, but be sure to talk to your doctor or another provider before taking these, as overuse can create other health problems.
Chronic inflammation is one of those stealthy health problems that makes itself known through a more obvious medical condition. Your best bet is not to wait to be diagnosed with an inflammation-related condition but to engage in healthy lifestyle strategies as early as possible to prevent inflammation from occurring. If you already have a condition like arthritis or diabetes, it’s never too late to make lifestyle changes and lower the impact the condition has on your life. Some physicians say that lifestyle medicine is the most powerful medicine of all, and it’s free!
For more expert guidance on menopause and healthy aging and to get our menopause app, download Midday.
Brittany Lubeck, RDN, MS is a Registered Dietitian Nutritionist with a Master of Science in Clinical Nutrition. She has training and experience working in a variety of clinical specialties and is now a nutrition writer and consultant. Brittany enjoys helping others sift through junk science and fad diets and believes that all foods fit. You can find Brittany online at Food Health.
Sign up for more unique women’s health content
By submitting this form, you agree to the Lisa Health Privacy Policy and Terms of Use
